Carotid artery blockage, clinically known as carotid artery stenosis, is one of the leading risk factors for stroke in the United States. But it’s also one of the most manageable vascular conditions when it’s caught and treated by the right specialists.
What Is Carotid Artery Blockage (Carotid Stenosis)?
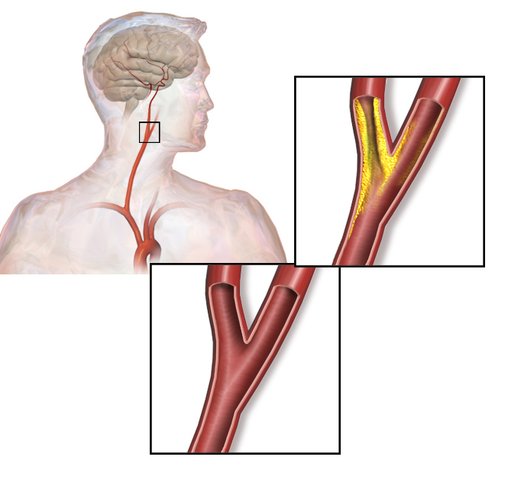
Your carotid arteries are the two large blood vessels that run along either side of your neck, supplying oxygen-rich blood to your brain. When these arteries become narrowed, usually from a gradual buildup of fatty plaque along the artery walls, blood flow to the brain is reduced. That narrowing is what doctors call carotid artery stenosis, or more plainly, a blockage or partial blockage of the carotid artery.
The degree of narrowing matters significantly. Mild or moderate stenosis may produce no symptoms at all and can often be managed without surgery. Severe stenosis, however, substantially raises the risk of stroke and typically requires intervention.
What Causes a Blocked Carotid Artery?
The most common cause is atherosclerosis, the same process responsible for most cardiovascular disease. Over time, cholesterol, calcium, and other substances accumulate along the inner walls of the arteries, forming plaques that stiffen and narrow the vessel. As the artery narrows, blood flow slows, and clots become more likely to form or break loose.
Several factors increase the likelihood of developing carotid artery disease:
- High blood pressure (hypertension)
- High cholesterol
- Type 2 diabetes
- Smoking
- Obesity or a sedentary lifestyle
- Age – risk increases notably after 65
- Family history of stroke, heart attack, or peripheral artery disease
Fibromuscular Dysplasia: A Less Common Cause
In some patients, more often younger women, carotid stenosis is caused not by plaque but by a condition called fibromuscular dysplasia (FMD). This is a structural abnormality in the wall of the artery itself that causes it to narrow or, in some cases, to develop a beaded appearance on imaging.
FMD is not related to cholesterol or lifestyle factors. It’s monitored and managed using similar standards as atherosclerotic stenosis, and most patients do well with conservative treatment and close surveillance.
What are the Warning Signs of a Blocked Carotid Artery?
Most people with carotid artery stenosis have no symptoms at all. The condition is often discovered incidentally during imaging for another issue or during a vascular screening exam. Finding the condition early allows for an opportunity to manage the disease before it causes harm.
People who experience symptomatic carotid disease should seek medical attention immediately. If you or someone near you experiences any of the following, call 911 and go to the nearest emergency room immediately:
- Sudden weakness or numbness on one side of the face, arm, or leg
- Sudden slurred speech or difficulty understanding what’s being said
- Sudden loss of vision in one eye sometimes described as a dark curtain briefly falling over your vision (this is called amaurosis fugax)
- Sudden, severe confusion or difficulty walking
These symptoms are signs of a stroke (cerebrovascular accident, or CVA) or a TIA (transient ischemic attack), often called a mini-stroke. A TIA causes the same symptoms as a stroke but resolves within minutes to hours. It should never be ignored: a TIA is a warning that a full stroke may be coming, and immediate evaluation is critical.
One important clarification: carotid artery stenosis does not typically cause dizziness, vertigo, blurred vision, or neck pain. If those are your primary symptoms, other conditions are more likely responsible, but a vascular evaluation can help rule out carotid disease as a contributing factor.
How Is Carotid Artery Disease Diagnosed?
Diagnosis is almost always imaging-based, since most patients don’t have symptoms that point directly to the carotid arteries. Two primary tools are used:
Carotid duplex ultrasound is typically the first step. It’s non-invasive, painless, and uses sound waves to produce real-time images of blood flow through the carotid arteries. It can identify narrowing, measure its severity, and assess plaque characteristics all without radiation or contrast dye.
CT angiography (CTA) provides a more detailed cross-sectional picture of the arteries and is often used when ultrasound findings suggest significant stenosis or when surgical planning is underway.
Based on imaging results, your vascular surgeon will classify the stenosis as mild, moderate, or severe, and that grading directly informs the treatment recommendation. Every patient’s situation is different, and your CVT vascular specialist will interpret your results in the context of your full medical history.
Treatment Options for Carotid Artery Blockage
Treatment for carotid artery stenosis is tailored to the severity of narrowing and whether symptoms are present. The goal in every case is the same: reduce stroke risk and protect your long-term health.
Medical Management for Mild to Moderate Stenosis
For many patients, particularly those with mild to moderate stenosis and no symptoms, medical management is the appropriate first approach. This typically includes:
- Antiplatelet therapy (such as aspirin or clopidogrel) to reduce the risk of clot formation
- Statin therapy to lower cholesterol and slow plaque progression
- Blood pressure management through medication and lifestyle changes
- Regular imaging surveillance to monitor the degree of stenosis over time
Reassuringly, many patients with carotid artery disease live well for years on medical management alone, especially when risk factors are actively controlled.
Carotid Endarterectomy (CEA): Surgical Plaque Removal
When stenosis is greater than 80%, or greater than 50% with symptoms, surgery is typically recommended. The gold standard procedure is carotid endarterectomy (CEA).
During a CEA, your vascular surgeon makes a small incision in the neck, carefully opens the carotid artery, and removes the plaque directly from the vessel wall. The artery is then repaired and blood flow restored. It’s a highly effective procedure with decades of clinical evidence supporting its ability to reduce stroke risk in appropriately selected patients.
CEA is performed under general or regional anesthesia, and most patients go home within one to two days of surgery.
Carotid Artery Stenting (CAS)
In select cases where surgery carries a higher risk due to prior neck surgery, radiation history, or certain cardiac conditions carotid artery stenting (CAS) may be recommended instead. This is a minimally invasive approach: using a small catheter threaded through a blood vessel, a mesh stent is placed inside the narrowed artery to hold it open and restore blood flow.
While stenting is used less frequently than CEA, it’s an important option for patients who aren’t ideal surgical candidates. The vascular specialists at CVT are experienced in both approaches and will help determine which is right for you.
Frequently Asked Questions About Carotid Artery Blockage
-
Can a blocked carotid artery cause a stroke?
Can a blocked carotid artery cause a stroke?
Yes. When the carotid artery is severely narrowed, blood flow to the brain is reduced, and plaque or clots can break free and travel to the brain, causing a stroke or TIA. Carotid artery disease is estimated to be responsible for up to 20% of all ischemic strokes. -
What does a carotid artery blockage feel like?
What does a carotid artery blockage feel like?
In most cases, it doesn’t feel like anything. Carotid stenosis is often completely asymptomatic. When symptoms do occur, they typically manifest as sudden neurological events: weakness on one side of the body, vision loss in one eye, or slurred speech. These require emergency care. -
Is carotid artery stenosis curable?
Is carotid artery stenosis curable?
The underlying atherosclerosis can’t be fully reversed, but carotid artery disease is highly manageable. With appropriate treatment, stroke risk can be significantly reduced and patients can live full, active lives. -
How serious is 50% carotid artery stenosis?
How serious is 50% carotid artery stenosis?
Moderate stenosis (around 50%) is taken seriously, particularly if accompanied by symptoms. Symptomatic stenosis at this level typically warrants surgical evaluation. Asymptomatic stenosis at 50% is usually managed medically and monitored closely with regular imaging. -
What is a TIA, and how does it relate to carotid disease?
What is a TIA, and how does it relate to carotid disease?
A transient ischemic attack (TIA), or mini-stroke, causes the same sudden neurological symptoms as a stroke but resolves on its own, usually within minutes. It’s a critical warning sign that the brain’s blood supply was briefly disrupted. Carotid artery disease is a common underlying cause. A TIA requires emergency evaluation, not a wait-and-see approach.
When to See a Vascular Specialist for Carotid Artery Disease
You don’t need to be experiencing symptoms to benefit from a vascular evaluation. Consider scheduling a consultation with a CVT vascular specialist if:
- You’ve been told you have plaque buildup or narrowing in your carotid arteries
- You have multiple cardiovascular risk factors: hypertension, diabetes, high cholesterol, a history of smoking
- You have a family history of stroke or heart disease
- You experienced a brief neurological event that has since resolved – don’t wait to follow up
If you’re currently experiencing stroke symptoms, go to the emergency room immediately. Your vascular surgeon will be consulted from there.
Get Expert Carotid Artery Care in Baton Rouge
Carotid artery disease is serious, but with the right care team, it’s also very manageable. The vascular surgeons at CVT Surgical & Vein Therapy Center specialize in the evaluation, diagnosis, and treatment of carotid artery stenosis, from medical management to surgical intervention.
If you’ve been told you have carotid artery narrowing, or if you want to understand your stroke risk better, we’re here to help. Contact CVT today to schedule a consultation with our vascular team in the Greater Baton Rouge area.