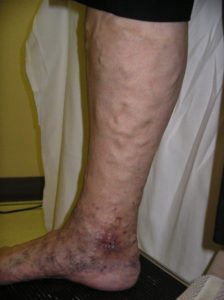
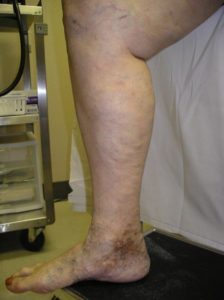
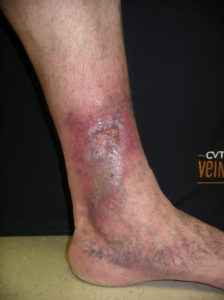
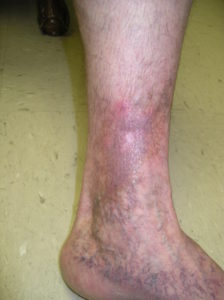
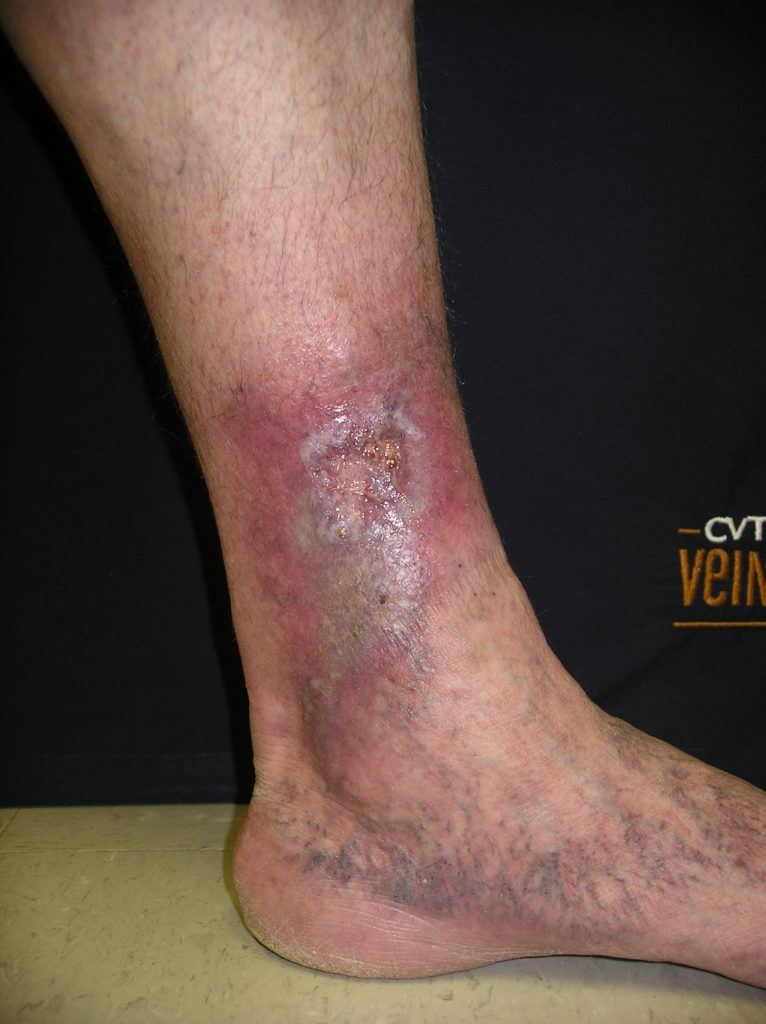
Venous Ulcer
A venous ulcer is a chronic, non-healing wound that typically develops on the lower leg due to poor blood circulation. Also called a venous stasis ulcer, this condition is most often caused by chronic venous insufficiency, a disorder in which the leg veins cannot properly return blood to the heart.
Venous ulcers are the most common type of leg ulcer. Without proper treatment, they can persist for months, worsen over time, and significantly impact mobility and quality of life.
What Is a Venous Ulcer?
A venous ulcer is an open sore that forms when blood pools in the lower legs due to malfunctioning vein valves. Over time, increased pressure in the veins damages the surrounding skin and tissue, leading to breakdown and ulcer formation.
What Causes Venous Ulcers?
The primary cause of a venous ulcer is chronic venous insufficiency (CVI). In healthy veins, small valves help push blood upward toward the heart. When these valves weaken or fail, blood flows backward and pools in the lower legs.
This pooling increases pressure inside the veins, leading to:
- Swelling
- Skin inflammation
- Tissue damage
- Eventual ulcer formation
Risk Factors for Venous Ulcers
You may be at higher risk if you have:
- Varicose veins
- A history of deep vein thrombosis (DVT)
- Obesity
- Prolonged standing or sitting
- Pregnancy
- Increasing age
Venous Ulcer Symptoms
Venous ulcer symptoms often develop gradually.
Common signs include:
- A shallow wound on the lower leg or ankle
- Irregular wound edges
- Swelling in the leg
- Brown or purplish skin discoloration
- Drainage or weeping
- Leg heaviness or aching
If you have a non-healing leg wound that has not improved in 2–4 weeks, it is important to seek evaluation from a vascular specialist.
How Venous Ulcers Are Diagnosed
Diagnosis begins with a physical examination. However, identifying the underlying circulation issue is essential for proper treatment.
Most patients undergo:
- Duplex ultrasound to evaluate blood flow
- Vascular imaging to assess vein function
- Circulation testing to rule out arterial disease
Accurate diagnosis ensures the correct treatment plan and improves healing outcomes.
Venous Ulcer Treatment Options
Effective venous ulcer treatment addresses both the wound and the underlying vein problem.
Compression Therapy
Compression therapy is the foundation of treatment. Special bandages or compression stockings:
- Improve blood return
- Reduce swelling
- Lower venous pressure
- Promote healing
Wound Care Management
Proper wound care may include:
- Debridement to remove damaged tissue
- Specialized dressings
- Infection prevention
- Ongoing monitoring
Treating the Underlying Vein Problem
To prevent recurrence, the faulty veins must be treated. Minimally invasive options may include:
- Endovenous ablation
- Sclerotherapy
- Other vein procedures that restore healthy circulation
- Debridement to remove damaged tissue
- Specialized dressings
- Infection prevention
- Ongoing monitoring
How Long Does a Venous Ulcer Take to Heal?
Venous ulcer healing time varies depending on:
- Size and severity of the ulcer
- Overall circulation health
- Patient compliance with compression therapy
- Presence of infection
With appropriate treatment, many venous ulcers improve within several weeks. However, untreated ulcers can persist for months or longer.
Recurrence is common if the underlying venous insufficiency is not corrected.
Preventing Venous Ulcers from Returning
Preventing recurrence requires long-term circulation management.
Key prevention strategies include:
- Wearing prescribed compression stockings
- Elevating legs regularly
- Maintaining a healthy weight
- Staying physically active
- Treating chronic venous insufficiency
Ongoing vascular care significantly reduces the likelihood of another ulcer developing.
When to See a Vascular Specialist for a Leg Ulcer
Venous ulcers are a sign of an underlying circulation problem that requires specialized care. You should seek medical care if:
- A leg wound does not heal within 2–4 weeks
- The wound becomes painful or infected
- You experience severe swelling
- You have a history of vein disease
CVT’s vascular specialists can determine whether the ulcer is venous, arterial, or related to another condition and develop a targeted treatment plan to restore healthy circulation and prevent further complications. Early treatment leads to better outcomes and faster recovery.
Frequently Asked Questions
-
What is the difference between a venous ulcer and an arterial ulcer?
What is the difference between a venous ulcer and an arterial ulcer?
Venous ulcers are caused by poor vein circulation and typically appear near the ankle. Arterial ulcers result from blocked arteries and are often more painful, appearing on the feet or toes. -
Can venous ulcers heal on their own?
Can venous ulcers heal on their own?
Most venous ulcers require medical treatment. Without addressing the underlying vein problem, they often persist or recur. -
Are venous ulcers dangerous?
Are venous ulcers dangerous?
If left untreated, venous ulcers can lead to infection, worsening tissue damage, and serious complications. -
Do compression stockings really help?
Do compression stockings really help?
Yes. Compression therapy is the cornerstone of venous ulcer treatment and helps improve blood flow and reduce swelling. -
Why do venous ulcers keep coming back?
Why do venous ulcers keep coming back?
Recurrence happens when chronic venous insufficiency is not treated. Correcting the underlying vein dysfunction reduces repeat ulcers.
Venous Therapy Results: Before and After